
Detect Pancreatic Cancer Early with A Pancreas Specialist
Pancreatic cancer often develops silently, showing few symptoms until it’s advanced. Early detection can make a crucial difference in treatment options and outcomes. Book a health review today to reveal any hidden tumours.
- Over 40 Years Of Combined Experience
- Minimally Invasive Pancreatic Surgery
- Same Day Appointments Daily Till 4pm
- Insurance and Medisave Claimable
Spot These Pancreatic Cancer Red Flags

Persistent pain in the upper abdomen that spread to the back

Ongoing loss of appetite

Yellowing of the skin or eye-whites (jaundice)

Darker urine and oily stools that are difficult to flush

Unintended weight loss

New-onset diabetes in adulthood
Early consultation with a pancreatic specialist allows for targeted scans, accurate diagnosis and prompt intervention, catching potential problems before they turn serious.

Dr Chan Chung Yip
MBBS, MMed(Surg), FRCS(Edin), MD, FAMS
Dr Chan Chung Yip is a senior general and pancreas surgeon, with domain expertise in a minimally invasive approach to complex pancreas operations.
With over 20 years of experience, he has managed a wide range of pancreatic conditions, including pancreatic cancer, pancreatic cysts, pancreatitis complex hepatopancreatobiliary (HPB) disorders.
Dr Chan shares his expertise regularly as author of numerous peer-reviewed publications in the field of pancreas surgery.
Languages Spoken:
- English
- Mandarin
- Cantonese
- Teochew / Hokkien

Dr Ho Choon Kiat
MBBS (Singapore), FRCS (Edin), FRCS (Glasg), M.Med (Surgery), FRCSEd (Gen), FAMS (Surgery)
Dr Ho Choon Kiat is a senior general and pancreas surgeon with a special interest in using minimally invasive / laparoscopic techniques to manage pancreas diseases.
He completed his surgical fellowship in pancreatic surgery and pancreatic cancer in Heidelberg, Germany in 2004. With a surgical practice spanning more than 20 years, Dr Ho has helped many patients with pancreatic diseases, including pancreas cancer, pancreatic cysts and pancreatic neuroendocrine tumours.
Dr Ho contributes to surgical education as an adjunct assistant professor at the Yong Loo Lin School of Medicine, and has authored numerous peer-reviewed publications as well as a book chapter in this field.
Languages Spoken:
- English
- Mandarin
- Cantonese
- Hokkien
The Courage Star (Singapore, 2003)
Daher Cutait Prize (ISUCRS, 2004)
Service Excellence Awards (Tan Tock Seng Hospital, 2003-04)
Sir Rodney Judson Prize (Royal Melbourne Hospital, 2006
Best Teacher Award (Tan Tock Seng Hospital, 2006-07)
Sir Rodney Judson Prize (Royal Melbourne Hospital, 2006
Best Teacher Award (Tan Tock Seng Hospital, 2006-07)
What is Pancreatic Cancer?
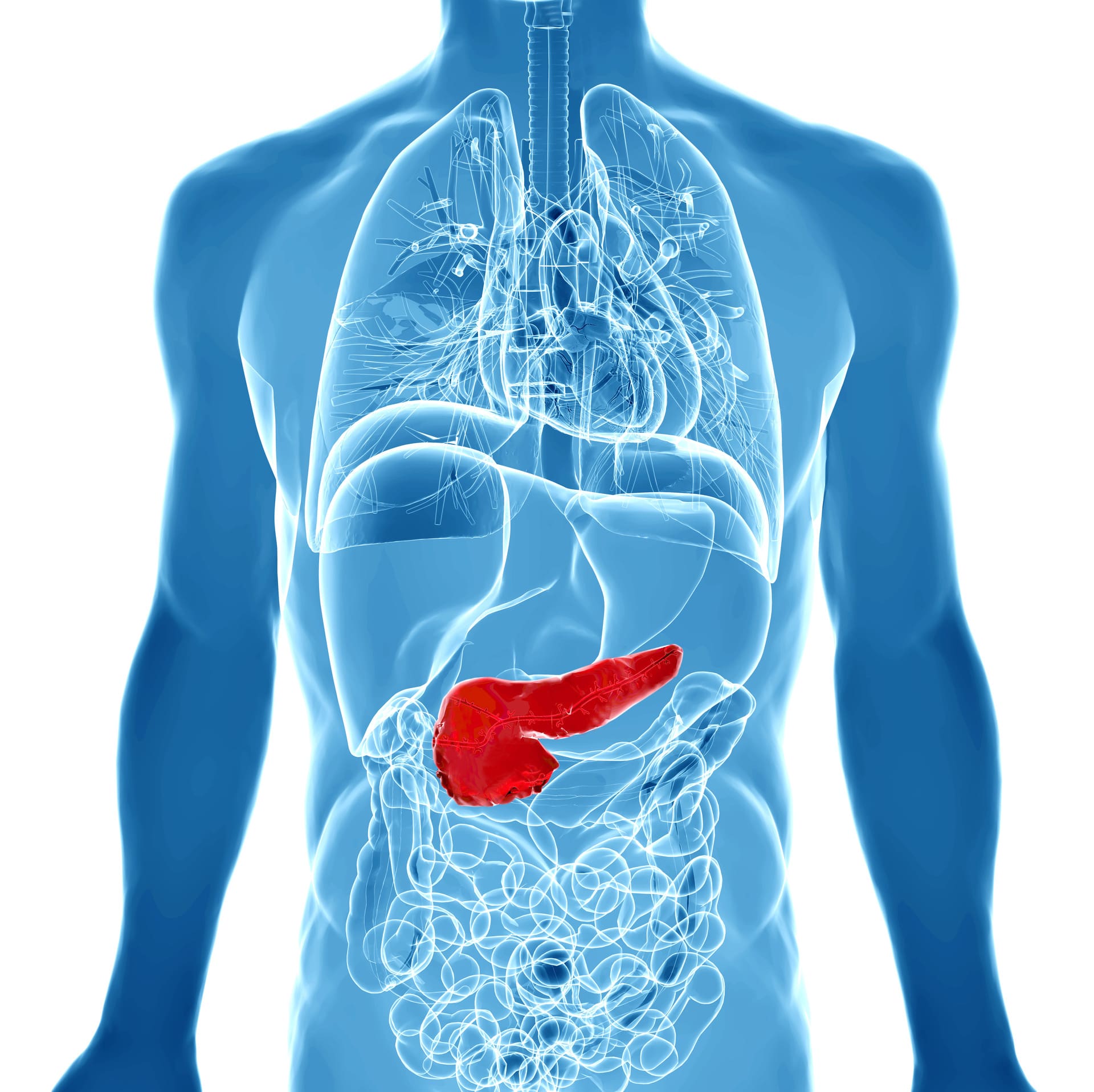
The pancreas sits high in the abdomen, tucked behind the stomach. Tiny ducts inside this gland carry digestive enzymes into the small intestine, while specialised cells produce hormones such as insulin to control blood-sugar levels.
Several tumour types can grow in the pancreas, but doctors usually use the term pancreatic cancer to describe malignancies of the cells lining the ducts. Pancreatic cancer is a very aggressive cancer, where only 1 out of 10 patients who have this disease can be treated by surgery.
When To Seek Pancreas Specialist

Ongoing Symptoms with Known Risks
You develop warning signs, such as unexplained upper-abdominal pain, jaundice, weight loss or persistent nausea, and have a family history of pancreatic disorders or cancer.

Unexpected Findings on Routine Tests
A medical check-up revealed something out of the ordinary:
• A raised tumour marker (especially CA 19-9), or
• A scan, ultrasound, CT or MRI, shows a suspicious growth in the pancreas.

Get a Second Opinion
You have been diagnosed with a pancreas condition and need an experienced specialist to help you understand your treatment options and plan your care with clarity.
After your pancreas specialist has assessed both the tumour location and your pancreas’s condition, they will recommend a suitable treatment plan.
Pancreatic Cancer Surgical Options
When disease is confined to the pancreas, surgery offers a high chance for long-term survival. The type of surgery depends on the location of the cancer in the pancreas.
Head of the Pancreas
-
Whipple Procedure (Pancreaticoduodenectomy)
Removes the pancreatic head, duodenum, gallbladder, part of the bile duct and sometimes a small section of stomach, then reconnects the digestive tract. -
Pylorus-Preserving Pancreaticoduodenectomy (PPPD)
A variation of the Whipple procedure that keeps the pylorus (the stomach’s outlet valve) intact if the tumour allows, helping food pass more naturally after surgery.
Body or Tail
-
Distal or Subtotal Pancreatectomy
Removes the affected segment in the body and tail of the pancreas and in some cases, the spleen, to clear wider disease spread.
Whole Gland or Multiple Areas Affected
-
Total Pancreatectomy
Rarely required, this removes the entire pancreas when the cancer involves the whole gland or multiple tumours are present.
4 Stages to Pancreatic Cancer Treatment
01
Step
Consultation and Planning
- Meet with your specialist — Dr Ho or Dr Chan — to review your scans, blood tests and medical history in detail.
- Talk through the treatment options together, so you know what will happen and can share any worries.
- Receive tips on fasting, exercise and medication tweaks to help you arrive for the surgery feeling prepared and supported.
02
Step
Pre-Surgery Preparation
- Complete CT or MRI scans to map the tumour, helping the team plan every detail.
- Blood tests and an anaesthetic review will be performed to confirm you’re ready for surgery.
- Medicine adjustments, such as fine-tuning diabetes treatment, are made under your doctor’s direction.
03
Step
During The Surgery
- You’ll be fully asleep under general anaesthetic.
- Your surgeon removes the diseased portion of the pancreas (plus nearby tissue if needed) and reconnects your digestive tract.
- Depending on the case, your surgeon will choose either a single open incision or a minimally invasive laparoscopic approach.
- The procedure can last several hours.
04
Step
Recovery After Procedure
- Recover in a high-dependence or ICU setting where nurses keep a close eye on pain, blood sugar and healing.
- Plan for a hospital stay of about 7–14 days for a Whipple procedure and 5–7 days for a Distal Pancreatectomy.
- While in hospital, you will receive pain relief and get support from physiotherapists to rebuild strength and ease breathing.
- Continue recuperating at home over the next weeks to months, where follow-up appointments to monitor progress may be arranged.
4 Stages to Pancreatic Cancer Treatment
01
Step
Consultation and Planning
- Meet with your specialist — Dr Ho or Dr Chan — to review your scans, blood tests and medical history in detail.
- Talk through the treatment options together, so you know what will happen and can share any worries.
- Receive tips on fasting, exercise and medication tweaks to help you arrive for the surgery feeling prepared and supported.
02
Step
Pre-Surgery Preparation
- Complete CT or MRI scans to map the tumour, helping the team plan every detail.
- Blood tests and an anaesthetic review will be performed to confirm you’re ready for surgery.
- Medicine adjustments, such as fine-tuning diabetes treatment, are made under your doctor’s direction.
03
Step
During The Surgery
- You’ll be fully asleep under general anaesthetic.
- Your surgeon removes the diseased portion of the pancreas (plus nearby tissue if needed) and reconnects your digestive tract.
- Depending on the case, your surgeon will choose either a single open incision or a minimally invasive laparoscopic approach.
- The procedure can last several hours.
04
Step
Recovery After Procedure
- Recover in a high-dependence or ICU setting where nurses keep a close eye on pain, blood sugar and healing.
- Plan for a hospital stay of about 7–14 days for a Whipple procedure and 5–7 days for a Distal Pancreatectomy.
- While in hospital, you will receive pain relief and get support from physiotherapists to rebuild strength and ease breathing.
- Continue recuperating at home over the next weeks to months, where follow-up appointments to monitor progress may be arranged.
Why Choose Our Pancreas Specialists in Singapore
Over 20 Years of Specialist Practice
Dr Chan and Dr Ho each bring more than 20 years of experience in pancreatic management and treatment.
Minimally Invasive Options
When tumour size and position permit, laparoscopic pancreatic surgery is offered, using smaller incisions for faster recovery and better outcomes.
End-To-End Care
From diagnosis to treatment and recovery, every stage of your care journey remains continuous and coordinated under one trusted team.
The surgeons at Nexus Surgical are part of the preferred panel of specialists for many local insurers, offering flexible payment arrangements for eligible patients.
Integrated Shield Plans






Third Party Administrators (TPA)






Costs & Funding Options
Pancreatic treatment procedures are MediSave-claimable, and many Integrated Shield or corporate plans can pay a share of the bill. For a figure tailored to your circumstances, speak with your hospital’s financial counsellor before booking.
In-Office
First Visit
$200 - $300
Repeat Visit
$150 - $250
Extended
$50 per block of 15 minutes
# > 30 for first visits
# > 15 for repeat visits
Out of Office
9:00 AM - 5:00 PM
$200 - $300
After 5:00 PM
$300 - $400
Hospital Inpatient
$200 - $400
Whipple operation or total pancreatectomy
S$22,400–S$33,600 (before GST)
Distal or subtotal pancreatectomy:
S$13,080–S$19,620 (before GST)
These numbers apply only to the surgeon’s professional fee. Your final hospital bill will also include:
- Your choice of hospital or ward
- Length of stay and post-operative support
- Charges for anaesthesia, imaging and laboratory tests
- Any co-payment, deductible and limits in your insurance plan
Book An Appointment Today
If you’ve noticed symptoms or want peace of mind about your pancreatic health, a specialist’s advice can make all the difference. Arrange a consultation with Dr Chan or Dr Ho in minutes by filling in the form or by phone.
Frequently Asked Questions on Pancreatic Cancer Surgery
Am I a candidate for pancreatic cancer surgery?
You’re eligible for surgery if scans show the tumour is confined to the pancreas and can be removed safely, and your overall health allows a major operation.
What are the risks and complications of pancreatic surgery?
Possible issues include infection, bleeding, leakage from re-joined intestines and delayed stomach emptying. Our surgical team monitors for these problems and treats them promptly.
How will surgery affect my digestion and blood sugar levels?
After a Whipple or similar procedure, you’ll experience an initial loss in appetite. Small, frequent meals can help while the body adjusts. Appetite usually improves within weeks to months.
What should I expect during my hospital stay after surgery?
You’ll start on IV fluids, then slowly resume eating and work with physiotherapists to regain strength. Most patients remain in hospital for about one to two weeks.
Mount Alvernia Hospital · Medical Centre A
-
820 Thomson Road
#03-03 Singapore
574623 - (65) 6353 4855
- (65) 6353 4106
Mount Elizabeth Orchard Medical Centre
-
3 Mount Elizabeth
#08-06 Singapore
228510 - (65) 6235 8633
- (65) 6235 5675
Mount Elizabeth Novena Specialist Centre
-
38 Irrawaddy Road
#08-43 Singapore
329563 - (65) 6570 2720
- (65) 6570 2710